As soon as you’ve implemented an EHR, the conversation will undoubtedly turn towards optimization. A 2017 study by KPMG in collaboration with CHIME reports that 38% of respondents ranked EMR/EHR optimization as their top choice for capital investments over the next three years. Your optimization 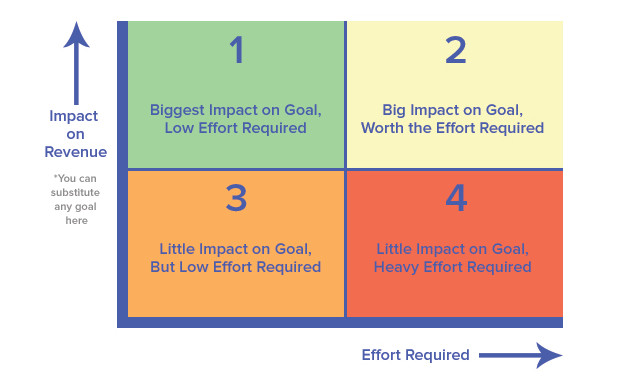 project begins by assembling a team that sets out to evaluate processes, identify features being underutilized, along with general enhancement opportunities. Using that initial analysis, a [sometimes] lengthy task list is compiled. These tasks will be ranked and sorted by estimating how much time each will take to implement, and the anticipated benefit afforded to your users or the organization at large.
project begins by assembling a team that sets out to evaluate processes, identify features being underutilized, along with general enhancement opportunities. Using that initial analysis, a [sometimes] lengthy task list is compiled. These tasks will be ranked and sorted by estimating how much time each will take to implement, and the anticipated benefit afforded to your users or the organization at large.
Prioritizing your Optimization
Next comes prioritization, which may involve a cost/benefit diagram or method of organizing from high value and low cost/effort to low value, high cost/effort. This sort of an approach allows you to pinpoint the low-hanging fruit (the high value / low cost items) in front of you, which should be executed first, and leaving behind some of the larger projects that may, or may not, offer tangible value. With this fairly standard approach, if your EHR has been in place for a decent length of time, you’ve probably snagged all of that low hanging fruit, right? Or have you?

The impending reality today with post-implementation Epic/EHR optimization is not only about checking as many of those high value, low cost items off your list, but also about solving the complexities present across your business domains, and in figuring out how to align optimization efforts with the aims and objectives related to delivering healthcare quality, achieving value-based reimbursement, reducing length-of-stay, and improving patient outcomes/experiences.
Finding the Low-Hanging Fruit
What if there was low-hanging fruit still on the vine but hidden from immediate view? What if you could study your ancillary departments such as radiology and lab, asking questions to identify when and where unnecessary tests might be being performed, leading to longer lengths-of-stay, avoidable bed days, and higher cost of admission? Maybe you perform duplicate tests as patients transfer between care areas, or perhaps you perform high-cost imaging studies as a first-line option despite literature suggesting that they provide no added value. These are Epic/EHR optimization opportunities that are ripe for the picking. You just have to know where to look.
We regularly find that low-hanging fruit does still exist for organizations, even after they have completed dedicated Epic optimization projects; and that this fruit, while sometimes more difficult to locate, offers far better returns. If you’d like to hear more about our methodology in locating these opportunities, and in taking a deeper dive into some of the benchmarks and metrics, give us a call (310-699-2017), or send our team an inquiry. We’d love to hear about your EHR optimization priorities.


